Welcome to WordPress. This is your first post. Edit or delete it, then start writing!
Lifetime Alcohol Use Linked to Higher Colorectal Cancer Risk!
Colorectal cancer remains one of the most common cancers worldwide, ranking as the third most frequently diagnosed cancer and the second leading cause of cancer-related deaths globally. While advances in screening and treatment have improved outcomes significantly over recent decades, the disease continues to affect hundreds of thousands of people each year. Recent research continues to shed light on modifiable risk factors that contribute to its development, offering hope that many cases might be prevented through lifestyle changes. Among these factors, alcohol consumption has emerged as a significant concern, with studies increasingly demonstrating that lifetime alcohol use—even at moderate levels—can substantially increase the risk of developing this disease.
Understanding the Connection Between Alcohol and Colorectal Cancer
The relationship between alcohol and colorectal cancer isn’t a new discovery. Medical researchers have suspected a link for decades, but recent large-scale epidemiological studies and meta-analyses have provided more nuanced and compelling insights into how cumulative alcohol exposure affects cancer risk over a lifetime. Unlike some risk factors that only matter in the present moment, the evidence suggests that your total lifetime alcohol consumption matters significantly when it comes to colorectal cancer. This cumulative effect means that decades of drinking, even at levels considered moderate or social, can create a substantial increase in risk.
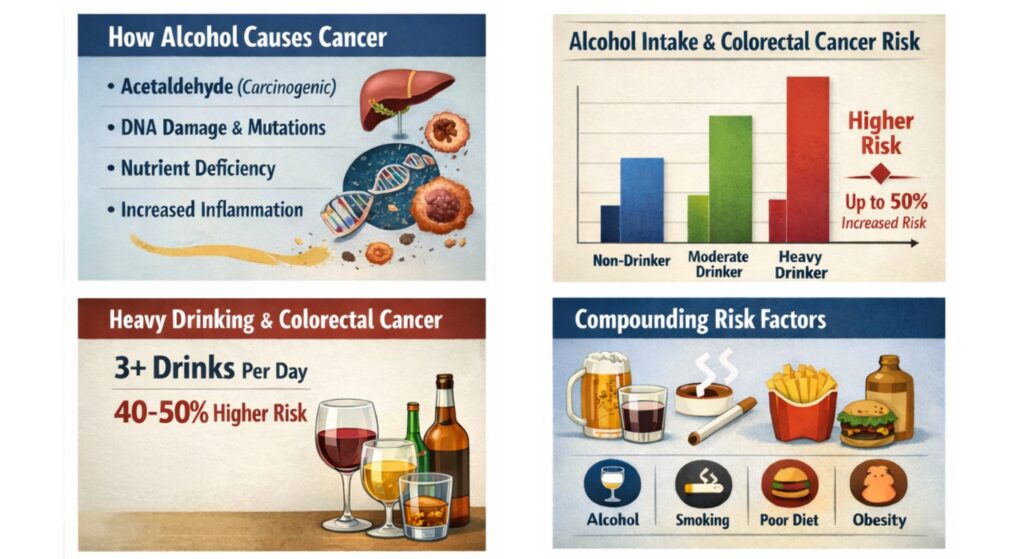
Research indicates that alcohol can promote cancer development through multiple biological pathways, making it what scientists call a “multi-mechanism carcinogen.” When you consume alcohol, your body metabolizes it primarily in the liver, but also in tissues throughout the body including the colorectal lining. This metabolism converts ethanol into acetaldehyde, a highly toxic compound that has been classified as a Group 1 carcinogen by the International Agency for Research on Cancer. Acetaldehyde can directly damage DNA and proteins within cells, creating mutations that can trigger cancerous cell growth. This damage, accumulated over time, creates an environment increasingly conducive to cancer development.
Additionally, alcohol can impair the body’s ability to absorb and utilize essential nutrients like folate, vitamin A, vitamin C, vitamin E, and carotenoids—all of which play protective roles against cancer through their antioxidant properties and involvement in DNA repair mechanisms. When alcohol interferes with these nutrients, it essentially removes some of the body’s natural defense systems against cancer. Furthermore, alcohol can increase levels of certain hormones linked to cancer risk and can act as a solvent, helping other carcinogenic substances penetrate tissues more easily. In the digestive tract specifically, alcohol can damage the mucosal barrier, increase inflammation, alter the gut microbiome in harmful ways, and promote the formation of reactive oxygen species that cause additional cellular damage.
The Dose-Response Relationship: How Much Is Too Much?
What makes the latest research particularly compelling is the clear dose-response relationship that has emerged from multiple large cohort studies: the more alcohol consumed over a lifetime, the higher the risk of colorectal cancer. This relationship appears to be nearly linear, meaning there’s no clear “safe” threshold below which risk disappears entirely. Studies have shown that even light to moderate drinking—often considered relatively safe and even promoted for potential cardiovascular benefits in the past—can incrementally increase risk when sustained over many years or decades.
Heavy drinkers face the most substantial risk elevation, with some studies suggesting that consuming three or more alcoholic drinks per day can increase colorectal cancer risk by 40-50% compared to non-drinkers or occasional drinkers. Some research has found even higher risk elevations for those who consume four or more drinks daily over extended periods, with risk increases approaching or exceeding 60% in certain populations. These are substantial elevations that place heavy alcohol consumption among the most significant modifiable risk factors for this disease.
However, moderate drinkers aren’t off the hook entirely. Consuming even one to two drinks daily over decades can measurably increase risk, with estimates typically ranging from 10-30% increased risk compared to non-drinkers. While this is a smaller elevation than that seen in heavy drinkers, it still represents a meaningful increase in absolute risk given how common colorectal cancer is in the population. The risk becomes particularly concerning when moderate drinking is combined with other factors like poor diet, obesity, smoking, or a sedentary lifestyle—all of which have their own independent associations with colorectal cancer.
Interestingly, the pattern of drinking may also matter. Some research suggests that binge drinking—consuming large amounts of alcohol in short periods—may be particularly harmful, potentially causing more acute damage to colorectal tissues than the same amount spread evenly over time. However, the evidence on drinking patterns versus total consumption remains an active area of research.


Why Lifetime Cumulative Exposure Matters More Than Current Habits
The concept of cumulative exposure is crucial to understanding alcohol’s role in colorectal cancer development. Your body doesn’t simply “reset” after periods of abstinence or reduced drinking. The cellular damage caused by alcohol, particularly the DNA mutations that accumulate in colorectal tissue over time, can persist even after you stop drinking. Damaged cells can continue dividing and passing mutations to daughter cells, creating clones of abnormal cells that may eventually progress to cancer.
This means that someone who drank heavily throughout their 20s, 30s, and 40s may still carry elevated risk even if they completely quit drinking in their 50s or 60s. While stopping alcohol consumption does provide benefits—preventing additional damage and allowing some repair mechanisms to function more effectively—it cannot completely erase the accumulated damage from decades past. This cumulative effect helps explain why colorectal cancer often develops later in life, typically after age 50, with incidence rates rising sharply with each subsequent decade. The decades of exposure create a foundation of cellular damage that eventually manifests as cancer.
This understanding also underscores why prevention efforts should focus on long-term patterns rather than just current behavior. Public health campaigns that encourage reduced alcohol consumption need to reach young adults, not just middle-aged or older individuals who may already have accumulated substantial exposure. Starting healthy habits early—or avoiding heavy alcohol consumption from the outset—can have profound effects on lifetime cancer risk.
Research examining former drinkers has found that while their risk remains elevated compared to lifetime non-drinkers, it does decrease over time after cessation. However, it may take many years or even decades for risk to approach that of non-drinkers, and in some cases, particularly for those with very heavy past consumption, risk may never fully return to baseline. This emphasizes both the importance of prevention and the value of quitting—while you can’t undo the past, you can prevent future damage.
Types of Alcohol: Does the Beverage Matter?
A common question among those trying to make healthier choices is whether the type of alcohol consumed makes a difference in cancer risk. This question often arises because of popular beliefs about red wine’s health benefits, stemming from observations about Mediterranean diets and the “French paradox.” While some studies have suggested that wine, particularly red wine, might have protective compounds like resveratrol, polyphenols, and other antioxidants, the evidence for colorectal cancer specifically indicates that the primary culprit is the alcohol (ethanol) itself, regardless of whether it comes from beer, wine, or spirits.
The ethanol content is what matters most from a cancer risk perspective, and all alcoholic beverages deliver this compound to your system when consumed. So while red wine might offer some cardiovascular benefits through its polyphenols and other bioactive compounds, these don’t appear to significantly offset the cancer risk associated with regular alcohol consumption. In fact, some large studies have found that the relationship between alcohol and colorectal cancer risk is consistent across beverage types when accounting for total ethanol consumed.
This doesn’t mean that all alcoholic beverages are identical in every health respect. They differ in caloric content, sugar levels, and the presence of various other compounds that might have health effects. However, when it comes specifically to colorectal cancer risk, the evidence points to alcohol content as the primary driver. A standard drink—whether it’s 12 ounces of beer, 5 ounces of wine, or 1.5 ounces of distilled spirits—contains roughly the same amount of pure alcohol (about 14 grams or 0.6 ounces of pure ethanol), and appears to carry similar risk implications for colorectal cancer.
Other Risk Factors That Compound the Problem
Alcohol doesn’t act in isolation when it comes to colorectal cancer risk. Its cancer-promoting effects can be amplified or compounded when combined with other lifestyle and genetic risk factors, creating particularly hazardous combinations that dramatically elevate risk beyond what any single factor would suggest.
People who drink heavily and also smoke face exponentially higher risks than those who only drink or only smoke. This synergistic effect occurs because tobacco and alcohol can work through overlapping mechanisms to damage DNA and promote cancer, while also impairing the body’s repair mechanisms in complementary ways. The combination has been described as creating a “perfect storm” for cancer development in the digestive tract.
Similarly, those who consume alcohol regularly while maintaining poor dietary habits—particularly diets low in fiber and high in processed meats, red meat, and refined carbohydrates—create a particularly dangerous environment for colorectal cancer development. Fiber helps move waste through the digestive system more quickly, reducing contact time between potential carcinogens and the colorectal lining. It also promotes a healthy gut microbiome and produces beneficial short-chain fatty acids during fermentation. When fiber intake is low and alcohol consumption is high, these protective effects are lost while harmful exposures increase.
Obesity is another significant compounding factor that interacts with alcohol consumption. Alcohol itself is calorie-dense, providing 7 calories per gram—nearly as much as fat and significantly more than carbohydrates or protein. These are often described as “empty calories” because they provide energy without essential nutrients. Regular alcohol consumption can easily contribute hundreds of calories per day, promoting weight gain over time. Obesity itself is an independent risk factor for colorectal cancer, likely through mechanisms involving chronic inflammation, insulin resistance, altered hormone levels, and effects on adipokines—hormones produced by fat tissue. The combination of alcohol’s direct cellular effects and its contribution to obesity creates a dual pathway to increased cancer risk.
Physical inactivity further compounds these risks. Regular physical activity appears to protect against colorectal cancer through multiple mechanisms, including effects on digestion time, inflammation, immune function, and hormone levels. When someone drinks regularly, maintains poor dietary habits, carries excess weight, and remains sedentary, they’ve essentially stacked multiple risk factors that work together to dramatically increase colorectal cancer risk.
Age is another consideration. While it’s not a modifiable risk factor, it does interact with lifetime alcohol exposure. As we age, our bodies become less efficient at repairing DNA damage and clearing damaged cells. This means that the accumulated damage from decades of alcohol consumption becomes increasingly likely to progress to cancer as we enter our 50s, 60s, and beyond.
Family history and genetic factors also play crucial roles. Individuals with a family history of colorectal cancer, particularly in first-degree relatives diagnosed at younger ages, already face elevated baseline risk. When these individuals also consume alcohol regularly over their lifetimes, they’re adding a substantial environmental risk factor on top of their genetic predisposition. Some genetic variants also affect how efficiently the body metabolizes alcohol, with some individuals accumulating more acetaldehyde and facing higher risk per drink consumed.
What This Means for You: Practical Implications and Recommendations
Understanding the link between lifetime alcohol use and colorectal cancer doesn’t necessarily mean you need to eliminate alcohol entirely, though complete abstinence would certainly minimize this particular risk factor. Rather, this knowledge should inform your choices and help you make decisions aligned with your personal health priorities and risk profile. Here are several practical takeaways based on the current scientific evidence:
Consider your cumulative exposure. If you’ve been a regular or heavy drinker for many years or decades, you may already have accumulated significant risk. While you cannot undo past consumption or reverse DNA damage that has already occurred, reducing or eliminating alcohol now can prevent further damage, allow your body’s repair mechanisms to work more effectively, and reduce your overall lifetime exposure. Every year of reduced consumption helps lower your risk trajectory going forward.
Moderation truly matters for ongoing exposure. If you choose to continue drinking, keeping consumption to minimal levels—ideally no more than a few drinks per week rather than daily consumption—can help limit your ongoing exposure and associated risk accumulation. Current guidelines from various health organizations suggest that if adults choose to drink, they should do so in moderation, typically defined as up to one drink per day for women and up to two drinks per day for men. However, even these levels carry some increased cancer risk when sustained over decades, so lower consumption is better from a cancer prevention standpoint.
Get screened according to guidelines or earlier if warranted. Colorectal cancer screening, typically recommended starting at age 45 for average-risk individuals (though some organizations recommend starting at 50), is crucial for early detection when cancer is most treatable. If you’ve had significant lifetime alcohol consumption, particularly when combined with other risk factors, discuss with your healthcare provider whether you should begin screening earlier than standard recommendations. Screening options include colonoscopy, which remains the gold standard, as well as stool-based tests and CT colonography. Don’t skip these screenings—they save lives by detecting cancer early or finding and removing precancerous polyps before they become cancer.
Address multiple risk factors comprehensively. Because alcohol’s effects are compounded by other lifestyle factors, improving your overall health profile can help offset some of the risk you may have accumulated. This means maintaining a healthy weight through balanced eating and regular physical activity, consuming a diet rich in fiber with plenty of fruits, vegetables, and whole grains while limiting red and processed meats, exercising regularly (at least 150 minutes of moderate activity or 75 minutes of vigorous activity per week), and absolutely not smoking or quitting if you currently smoke. Each of these changes independently reduces colorectal cancer risk, and together they can substantially lower your overall risk profile.
Be honest with your healthcare provider about your drinking history. When discussing your health history with your doctor, be forthcoming and accurate about your lifetime alcohol consumption patterns, including both current habits and past periods of heavier drinking. Many people underreport their alcohol consumption due to embarrassment or not wanting to be judged, but accurate information is essential. This information helps your doctor assess your comprehensive risk profile, recommend appropriate screening schedules, and provide personalized guidance. Remember that healthcare providers are there to help, not judge, and they’ve heard it all before.
Consider your family history and genetic risk. If you have a family history of colorectal cancer or other risk factors that increase your baseline risk, be particularly cautious about alcohol consumption. When you start with elevated genetic risk and add environmental risk factors like alcohol, you’re multiplying your chances of developing the disease. Some individuals may benefit from genetic counseling or testing, particularly if they have multiple family members affected by colorectal or other cancers at young ages.
Stay informed about evolving guidelines. Our understanding of alcohol and cancer risk continues to evolve as new research emerges. Public health recommendations have become increasingly conservative regarding alcohol consumption as evidence of cancer risks has strengthened. Stay informed about current guidelines and be willing to reassess your habits as new evidence emerges.
The Bigger Picture: Alcohol and Overall Health
The connection between lifetime alcohol use and colorectal cancer risk is part of a broader conversation about alcohol and health that has evolved significantly in recent years. While moderate drinking has sometimes been promoted for potential cardiovascular benefits based on observational studies, the evidence for cancer risk—including not just colorectal cancer but also liver, breast, esophageal, and other cancers—is increasingly clear and concerning. Recent analyses suggest that no amount of alcohol is completely without risk, and even light drinking carries some increased cancer risk when sustained over a lifetime.
This doesn’t mean everyone who drinks will develop cancer, nor does it mean that alcohol is the sole cause of colorectal cancer—genetics, diet, obesity, physical activity levels, and other environmental factors all play important roles in determining who develops the disease. However, it does mean that alcohol consumption is a significant modifiable risk factor that individuals can control through their choices. When you consider that alcohol also contributes to liver disease, cardiovascular problems at higher doses, accidents, injuries, addiction, and numerous other health issues, the overall risk-benefit calculation looks quite different from how it might have been presented in the past.
As research continues to illuminate these connections, public health messaging is evolving to reflect a more cautious and realistic stance on alcohol consumption. Many countries have revised their drinking guidelines downward in recent years as the evidence on cancer risk has strengthened. Understanding that your lifetime cumulative exposure matters empowers you to make informed decisions about your health, both today and for your future, weighing the social and personal benefits you may derive from drinking against the very real health risks it carries.
Conclusion: Knowledge Is Power for Prevention
The key message emerging from decades of research is clear: when it comes to colorectal cancer risk, your lifetime relationship with alcohol matters significantly. The damage accumulates over years and decades, creating an elevated risk that persists even after you stop drinking, though quitting certainly helps prevent additional damage. Whether you’re currently a regular drinker, an occasional drinker, or simply reflecting on past habits, this knowledge provides an opportunity to reassess your choices and take proactive steps to protect your long-term health.
For those who have consumed significant amounts of alcohol over their lifetimes, the message isn’t one of doom but rather one of empowerment through action. While you cannot change the past, you can change your future trajectory through screening, lifestyle modifications, and reduced or eliminated alcohol consumption. For younger individuals who may be establishing their lifelong habits, understanding these risks early provides an opportunity to make informed choices that will pay health dividends for decades to come.
The good news is that colorectal cancer is highly preventable through screening and lifestyle modification, and it’s highly treatable when caught early. By understanding the role of alcohol as one important risk factor among several, taking action to minimize your ongoing exposure, addressing other modifiable risk factors, and participating in recommended screening, you can substantially reduce your risk of developing this common but largely preventable disease. Your health is worth the effort, and the choices you make today can profoundly impact your wellbeing for years to come.