Welcome to WordPress. This is your first post. Edit or delete it, then start writing!
The Silent Threat That Doubles a Mother's Stroke Risk During Pregnancy!

A Wake-Up Call for Expecting Mothers
For decades, pregnancy has been celebrated as one of the most beautiful and transformative phases of a woman’s life. And it is. But beneath that beauty lies a set of biological changes that, for some women, quietly raise the stakes in ways most people never consider. Stroke — a condition most people associate with older adults — can strike during pregnancy or in the weeks immediately following childbirth. And for women who have already experienced a stroke once, the danger is dramatically higher than anyone previously understood.
A preliminary study presented at the American Stroke Association’s International Stroke Conference 2026 has shed startling new light on this risk. The findings don’t just offer a warning — they demand a fundamental rethinking of how we monitor and protect pregnant women with a history of stroke.
“Controlling blood pressure and other stroke risks before and after delivery, responding immediately to stroke warning signs and providing timely treatment can help save lives and improve outcomes for mothers and their babies.”
— Dr. Eliza Miller, Associate Professor of Neurology, University of Pittsburgh


What the 2026 Study Found
The research examined data from 220,479 completed pregnancies spanning from January 2015 to February 2025. Of these, 1,192 women had a documented history of ischemic stroke — the kind caused by a blood clot blocking blood flow to the brain. What the study uncovered was sobering: 415 of those women, or 34.8%, suffered a recurrent ischemic stroke during pregnancy or within the first six weeks after delivery.
To understand just how alarming that number is, consider the comparison. Among women without a prior stroke, the rate of ischemic stroke during pregnancy or postpartum was just 0.34%. Women with a previous stroke were, statistically speaking, more than a hundred times more likely to experience the same devastating event again — at one of the most vulnerable moments of their lives.
The study further identified two key factors that compounded the danger for women with a prior stroke history: a previous heart attack and obesity. Both conditions were independently linked to a higher chance of recurrent ischemic stroke during pregnancy or the early postpartum window.

Why Does Pregnancy Increase Stroke Risk?
To understand why pregnancy puts women at higher risk for stroke, you need to understand what pregnancy does to the body at a biological level. During pregnancy, the body undergoes massive hormonal, cardiovascular, and metabolic changes — all designed to support the growing baby. But some of those changes, while necessary, also create conditions that make blood clots more likely to form.
Pregnancy shifts the body into what scientists call a “hypercoagulable state.” This means the blood becomes more prone to clotting. This is actually a survival mechanism — it helps reduce bleeding during and after childbirth. But for women whose vascular system is already under stress from a prior stroke, this natural clotting tendency can become dangerous. Blood pressure rises, blood volume increases, and venous flow slows — all of which can tip the balance toward a stroke event.
According to the American Heart Association’s 2026 Heart Disease and Stroke Statistics, nearly half of all pregnancy-associated stroke hospitalizations occur in the setting of hypertensive disorders. Conditions like preeclampsia and eclampsia — where blood pressure spikes dangerously — are among the strongest risk factors. And for women who already carry a prior stroke on their medical history, these pregnancy-driven changes don’t just add risk. They amplify it.


⚠️ Who Is Most at Risk?
While stroke during pregnancy is rare overall — occurring in roughly 20 to 40 out of every 100,000 pregnancies — certain women face a much higher likelihood. If you or someone you know falls into any of these categories, early and proactive care is critical.
- →Women with a previous ischemic stroke
- →Those with chronic hypertension or preeclampsia
- →Women with a history of heart attack
- →Those over 35 years of age (advanced maternal age)
- →Women with obesity, diabetes, or clotting disorders
- →Those with a history of migraines with aura
What Experts Are Now Recommending
The American Heart Association released a landmark scientific statement in January 2026, endorsed by the American College of Obstetricians and Gynecologists, that outlines a comprehensive approach to preventing and treating stroke in pregnant and postpartum women. The guidance is clear: prevention must start before conception.
For women with a history of stroke who are planning a pregnancy, experts are now recommending structured preconception counseling as a mandatory first step. This includes a thorough review of all medications — some commonly used stroke medications, like statins and ACE inhibitors, are dangerous during pregnancy and must be stopped or switched well before conception. Blood pressure must be brought under tight control, and anti-clotting medication plans need to be carefully tailored for the pregnancy journey ahead.
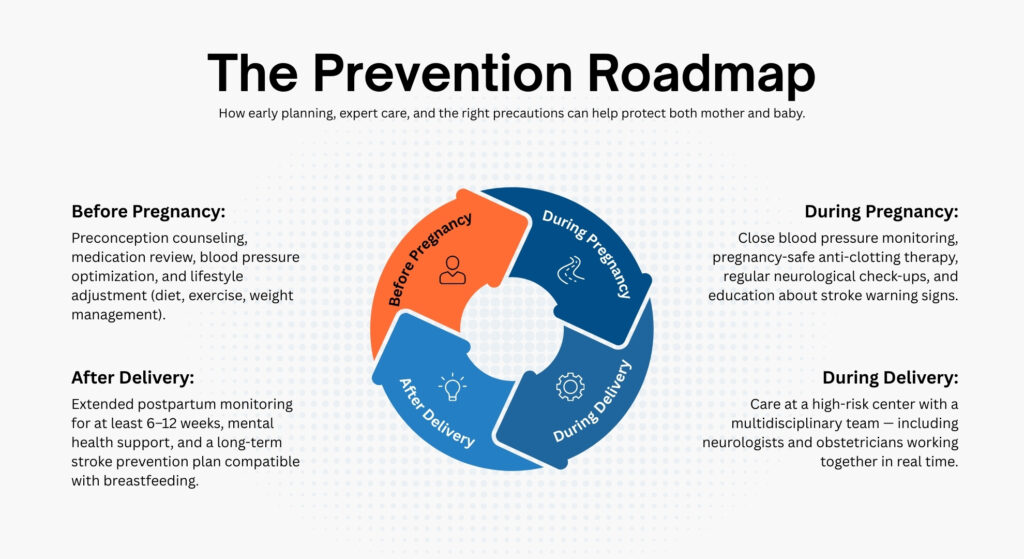
The Gap in Research — and Why It Matters
One of the most troubling aspects of this story isn’t the risk itself — it’s how long the medical world has been in the dark about it. For decades, pregnant and postpartum women have been excluded from clinical trials. The reasoning was ethical: researchers didn’t want to expose the fetus to experimental treatments. The result? A massive gap in the evidence base that healthcare providers rely on to make life-or-death decisions.
The 2026 AHA statement explicitly calls for inclusive clinical trials — studies that bring pregnant women into the research process so that real, evidence-based treatments can be developed. Until those trials happen, doctors will continue to rely on observational data, which, while valuable, cannot replace the gold standard of controlled research.
Dr. Eliza Miller and her colleagues wrote it plainly: “Continued research, including inclusive clinical trials, is urgently needed to refine stroke risk assessment, to expand treatment options, and to improve maternal outcomes.” The message is urgent. The gap is wide. And the lives at stake make closing it a moral imperative.
Recognizing the Warning Signs
Whether you are pregnant, postpartum, or planning a pregnancy, knowing the warning signs of a stroke could save your life — or someone you love. Stroke is a time-critical emergency. Every minute of delayed treatment increases the chance of permanent brain damage.
- Face Drooping
Ask the person to smile. Does one side of their face droop or feel numb? An uneven smile is a red flag.
- Arm Weakness
Ask them to raise both arms. Does one arm drift downward or feel weak and unable to stay up?
- Speech Difficulty
Is their speech slurred, strange, or difficult to understand? Ask them to repeat a simple sentence.
- Time to Call
If any of these signs are present, call emergency services immediately. Time is brain — every second counts.
What This Means Going Forward
The 2026 stroke-in-pregnancy findings represent more than just a scientific discovery. They represent a turning point in how medicine approaches maternal health. For too long, stroke in pregnancy has been treated as an afterthought — a rare event that didn’t warrant the same urgency as other pregnancy complications. That narrative is changing.
With the American Heart Association now issuing formal guidance, the American Stroke Association highlighting these findings at its flagship conference, and a growing body of research demanding inclusive clinical trials, the stage is set for real, systemic change. Hospitals will need to build specialized pathways for high-risk pregnancies. Obstetricians will need to collaborate more closely with neurologists. And women themselves — especially those with a prior stroke — will need to be empowered with the information and care they deserve.
Pregnancy is a time of hope. It should also be a time of safety. The research of 2026 is making it clear that for millions of women, achieving that safety requires action — from the medical system, from policymakers, and from each of us who understands the weight of what these numbers truly mean.